When someone tells you that you need ICSI, it’s natural to feel confused. Your first instinct might be to think: Wait, isn’t that just a fancy name for IVF?
The honest answer is no—but I understand why you’d think that.
ICSI and IVF aren’t the same thing. Think of it this way: IVF is the overall fertility treatment process. ICSI is one specific technique used during that process. For some couples, ICSI makes all the difference. For others, it won’t help at all.
Dr. Mohit Saraogi puts it simply: “ICSI solves one problem—when a man’s sperm can’t fertilize an egg on its own. But it’s not a cure-all. We only recommend it when the lab results show it’ll actually help your situation.”
Over the years, we’ve worked with hundreds of couples dealing with male factor infertility. The ones who do best are the ones who truly understand what ICSI is, why they might need it, and what to realistically expect. That’s what this guide is about. We’ll walk you through what ICSI actually does, when you genuinely need it, what it costs, and how it changes your chances of success. No jargon. No overselling. Just the facts.
Understanding IVF & ICSI: Let's Clear Up the Confusion
ICSI and IVF are not two different treatments competing with each other. That’s the biggest misconception we see.
Here's what actually happens
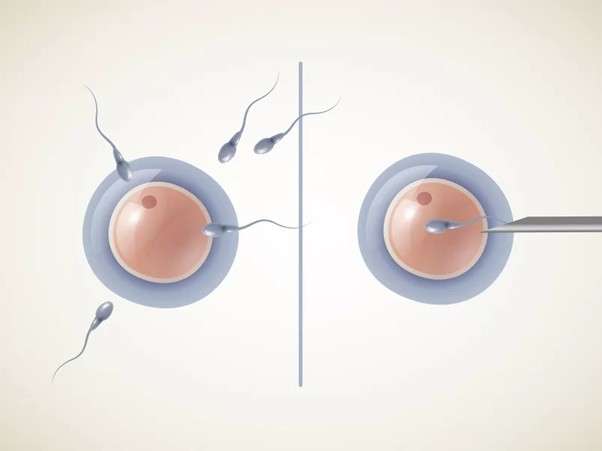
In regular IVF, here's the basic process:
Your eggs are collected. Your partner’s sperm is collected. We put them together in a dish and let nature do its thing. The sperm finds the egg, enters it, and fertilization happens naturally—just like it would in your body. Then we watch the embryo develop over the next five days. With ICSI, almost everything is the same—except for one crucial moment. Instead of letting sperm find the egg naturally, we do something very specific: We take one single healthy sperm and inject it directly into the egg using a microscopic needle. That’s it. The rest of the process unfolds exactly like regular IVF.
A simple way to think about it:
Imagine a locked room with an egg inside. In regular IVF, we unlock the door and let sperm swim in on their own. With ICSI, we unlock the door, pick one sperm, and physically guide it inside. The result—a fertilized egg—is the same either way. The method is just different.
Here's the critical point that changes everything:
ICSI is only helpful if your sperm has specific problems preventing natural fertilization. If your sperm is healthy and swimming well, ICSI won’t improve anything. It’ll just add cost without benefit.
This is exactly why understanding your semen analysis matters so much. Those numbers tell us whether you actually need ICSI or if regular IVF will work fine.
When Do You Actually Need ICSI? (Here's What Your Numbers Mean)
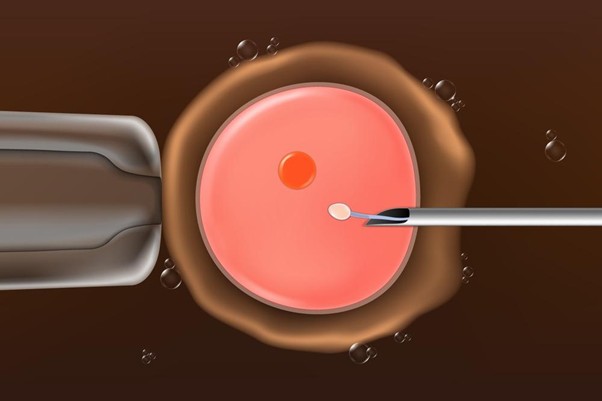
Not everyone needs ICSI. But certain sperm issues make it essential.
Low Sperm Count (Below 15 Million Per Milliliter)
With low count, few sperm can reach the egg naturally. Regular IVF fertilizes only 20-30% of eggs. ICSI fertilizes 50-60% of the same eggs. We inject sperm directly—no swimming required.
Slow-Moving Sperm (Motility Below 40%)
If sperm can’t swim well, they struggle to reach the egg. ICSI bypasses this problem completely. We deliver the sperm directly to the egg.
Abnormally Shaped Sperm (Over 96% Abnormal)
When most sperm have abnormal shapes, natural fertilization is unlikely. ICSI lets us find and inject the few healthy sperm available.
Previous Fertilization Failure
If less than 2% of your eggs fertilized in a previous IVF cycle, something blocked natural fertilization. ICSI removes that barrier. It’s the logical next step.
High DNA Fragmentation
Sometimes sperm look normal, but their DNA is damaged. This causes fertilization failure or poor embryo development. ICSI combined with other strategies can help.
Ejaculation Problems
Retrograde ejaculation, blocked ducts, or no ejaculation mean sperm must be retrieved directly from the testicle (TESE procedure). With limited sperm available, ICSI prevents waste and maximizes fertilization.
When You Probably DON'T Need ICSI
If your semen analysis shows normal results—normal sperm count (over 15 million/ml), normal movement (over 40% forward motion), and normal shape (less than 96% abnormal)—you don’t need ICSI. Your sperm already fertilize eggs naturally. If your infertility is a female factor issue (your partner’s age, endometriosis, blocked tubes, or low ovarian reserve), ICSI won’t help because the problem isn’t sperm fertilization. Similarly, if your infertility is unexplained but your sperm parameters are normal, ICSI doesn’t improve your odds. Some clinics recommend ICSI to every male partner anyway—because they can charge more. Don’t fall for it. Ask your doctor to explain specifically why ICSI is recommended for your numbers, not as a blanket recommendation.
Here’s the truth: Your semen analysis numbers matter enormously. Two patients with similar sperm counts might get completely different ICSI recommendations based on other parameters like motility or morphology. Patient A with a count of 40 million/ml, 55% motility, and 4% normal morphology might need ICSI. Patient B with 50 million/ml, 60% motility, and 3% normal morphology might not. The difference? Patient A’s numbers cross a threshold where ICSI becomes genuinely beneficial. Patient B’s don’t. This is why getting your actual numbers and understanding them is critical. Ask your doctor: “Based on these specific numbers, why do I need ICSI?” If they can’t give you a clear answer tied to your results, get a second opinion.
The ICSI Process: What Actually Happens (Step by Step)
Days 1-12: Ovarian Stimulation
You take hormone injections to help your ovaries produce multiple eggs. You’ll have ultrasounds to monitor progress. You might experience bloating or mild discomfort—normal side effects. This phase is identical to regular IVF.
Day of Egg Retrieval
Two things happen simultaneously: Your eggs are collected through a needle-guided ultrasound procedure (takes 15 minutes, you’re sedated). Your partner provides a fresh semen sample in a private room at the clinic. Timing matters—the sample must be fresh for the lab.
In the Lab: ICSI Happens Here (2-4 Hours)
The embryologist examines your partner’s semen, selects one healthy sperm, and injects it directly into each egg using a microscope. This is the only difference from regular IVF—instead of letting sperm fertilize eggs naturally, we do it for them. They check for fertilization 16-18 hours later
Days 1-5: Embryo Development
Your embryos develop normally: Day 1 (2 cells), Day 2 (4 cells), Day 3 (8 cells), Day 5 (blastocyst). ICSI doesn’t change how embryos develop. Success now depends on embryo quality and genetics.
Day 5-6: Embryo Transfer
One or two embryos are transferred into your uterus using a thin catheter. It feels similar to a Pap smear—uncomfortable but not painful. The embryos don’t know how they were fertilized.
Days 7-12: The Wait
You go home and wait. Progesterone support continues. This waiting period is emotionally tough—that’s normal. Stay realistic and lean on your clinic’s support.
Day 12-14: Pregnancy Test
A blood test checks hCG levels to confirm if the embryo has implanted. If positive, follow-up ultrasounds confirm a healthy pregnancy. If negative, your clinic discusses the next steps.
Timeline: Start to Answers = 26 Days
Days 1-12 (Stimulation) → Day 13 (Retrieval) → Days 14-18 (ICSI & Development) → Days 19-20 (Transfer) → Days 21-26 (Wait & Test)
Conclusion
ICSI isn’t a miracle treatment; it’s a targeted solution for male factor infertility. If your sperm count is low, motility is poor, or you’ve experienced fertilization failure before, ICSI can dramatically improve your chances of pregnancy. But if your sperm is healthy, adding ICSI just wastes money. The key is getting proper testing and choosing a clinic that specializes in male factor cases, not one that recommends ICSI to everyone. At Saraogi Hospital, we review your specific semen analysis numbers and recommend ICSI only when it will genuinely help your situation.
Don’t let confusion about ICSI delay your fertility journey. Understanding whether you need ICSI requires clear answers based on your actual test results. If you’re unsure whether ICSI is right for you, book a consultation with our male factor fertility specialists today. We’ll analyze your semen parameters, explain your options honestly, and create a personalized treatment plan. Your path to parenthood starts with the right diagnosis and the right clinic.
Frequently Asked Questions
Is ICSI the same as IVF?
No. IVF is the overall process. ICSI is one technique used during IVF. Every ICSI cycle involves IVF, but not every IVF cycle uses ICSI. It depends on your sperm.
Does ICSI cost a lot more?
It adds ₹15,000-25,000 to your IVF cost. So if IVF costs ₹2 lakhs, ICSI brings it to ₹2.15-2.25 lakhs. It’s worth the money if you need it, but wasteful if you don’t.
If I do ICSI, will I definitely get pregnant?
No. ICSI solves fertilization problems. But pregnancy involves many other factors: egg quality, embryo development, uterine health, implantation. ICSI improves your odds for the fertilization step. Everything else is separate.
Can the injection damage my eggs?
Very rarely. Less than 5% of eggs suffer damage from injection. Most fertilize and develop normally. Our embryologists minimize this risk through training and care.
How long does the actual ICSI procedure take?
The injection process takes 2-4 hours depending on egg count. You’re not awake during this—you’re recovering from your egg retrieval. The embryologist does all the work.
Should I do ICSI even if my sperm looks borderline normal?
Ask your doctor to explain why, based on your specific numbers. If sperm parameters are truly normal, ICSI won’t help. Some clinics recommend it anyway for profit. Don’t assume—question it.
If my first IVF cycle had zero fertilization, should I definitely do ICSI next time?
Very likely yes. Zero fertilization suggests sperm couldn’t fertilize naturally. ICSI directly solves this. But get your semen analysis checked first. Sometimes the problem is egg quality, not just sperm.
Can I do IVF without ICSI if my sperm count is low?
Technically yes, but not recommended if count is very low. Low count means few sperm available. Hoping one naturally finds and fertilizes an egg leaves you with terrible odds. ICSI gives you reasonable chances.
Is ICSI better than regular IVF?
For male factor: Yes, absolutely. For normal sperm: No, they’re equal. It entirely depends on your diagnosis.
How much sperm do you need for ICSI to work?
Just one healthy sperm per egg. Even if your count is extremely low—like 1 million or less—if we can find one good sperm, ICSI works beautifully. That’s actually the power of ICSI.
Can ICSI make embryo quality better?
No. ICSI helps sperm get into the egg. Embryo quality depends on the genetics of the egg and sperm. ICSI doesn’t change that. A healthy embryo from ICSI is no different from one created through regular IVF.
Is ICSI safe for the baby?
Yes. Decades of research confirm this. Children born from ICSI have identical health outcomes to naturally conceived children. No increased risks. No genetic changes.

