Successful Live Birth After Donor Egg IVF, Hysteroscopic Adhesiolysis, and Laparoscopic Cervical Cerclage in a Woman with Cervical Amputation and Prior IUFD
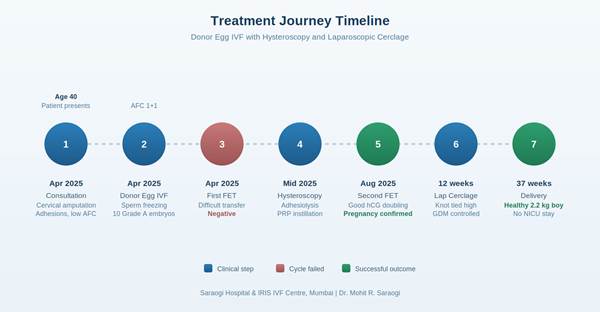
A 40-year-old woman married for 18 years came to Saraogi Hospital, Mumbai after losing both her daughters in a road accident and an intrauterine foetal death at 8 months in her most recent pregnancy. She had cervical amputation from an unsupervised rural procedure, severe intrauterine adhesions, and a failed IVF cycle elsewhere. Dr. Mohit R. Saraogi managed the case with donor egg IVF, hysteroscopic adhesiolysis with PRP, and an elective laparoscopic cervical cerclage. She delivered a healthy 2.2 kg male baby at 37 weeks with no NICU admission.
PATIENT PROFILE
| AGE | 40 years |
| GENDER | Female |
| HUSBAND’S AGE | 54 years |
| MARRIED SINCE | 18 years |
| CITY | Rural patient, referred to Mumbai |
| PRESENTING COMPLAINT | Secondary infertility after IUFD, prior IVF failure, chronic pelvic symptoms |
| DIAGNOSIS | Cervical amputation, intrauterine adhesions, low ovarian reserve (AFC 1+1), advanced maternal age |
| DATE OF PROCEDURE | April 2025 to delivery |
| OUTCOME | Healthy live birth at 37 weeks |
THE PROBLEM
Her story was heavy before she even sat down in the clinic. Two daughters lost in a road accident. A pregnancy one year before her visit that ended in intrauterine foetal death at around 8 months of gestation, followed by a vaginal delivery. Since then, trying to conceive again had become the only thing that mattered.
Her medical history was complicated and partly unknown even to her. After her last delivery 8 to 9 years ago, she had severe bleeding in her village. A procedure was performed on her cervix, not in a hospital, not by a qualified doctor, and without any records. She had lived since then with a constant feeling of something coming out from her vagina, suggesting uterine prolapse. One IVF cycle done elsewhere had already failed. By the time she reached Saraogi Hospital in April 2025, she was 40, carrying loss on every front, and running out of time.
CONSULTATION AND TREATMENT PLAN
WHAT WAS ASSESSED DURING THE CONSULTATION
Dr. Mohit R. Saraogi conducted a full evaluation before planning treatment:
- Vaginal ultrasound showed the cervix was not visible at all
- Per speculum examination confirmed cervical amputation, not a formal Fothergill procedure, just a surgical cut
- External os was visible, and uterine sounding confirmed an easy entry into the uterus with no cervix as a structural barrier
- Antral follicle count was 1 on each side, indicating diminished ovarian reserve
- History of one failed IVF cycle outside reviewed
- Husband’s availability confirmed for sperm freezing due to frequent travel between the village and Mumbai
- Psychological state assessed given the cumulative pregnancy loss history
WHY THIS TREATMENT APPROACH WAS CHOSEN
Donor egg IVF was recommended because the patient’s AFC was 1+1 and one self-egg IVF cycle had already failed. Own-egg success at age 40 with this reserve was clinically unviable
- Sperm and embryo freezing was done simultaneously to avoid scheduling issues caused by the husband’s travel
- Hysteroscopy with PRP instillation was planned after the first transfer failure to manage fundal adhesions and improve endometrial receptivity
- Laparoscopic cervical cerclage (lap surclash) was pre-planned as elective post-conception, because the absence of a functional cervix meant a normal pregnancy could not reach term without surgical reinforcement
- Blastocyst-stage frozen embryo transfer was chosen over fresh transfer to allow full endometrial preparation and cavity optimisation
PROCEDURE ILLUSTRATION
The patient underwent donor egg IVF followed by frozen embryo transfer. The diagram below shows the standard IVF workflow. In this case, donor eggs were used due to the patient’s diminished ovarian reserve (AFC 1+1), and embryos were transferred after cavity optimisation through hysteroscopic adhesiolysis and PRP instillation.
PROCEDURE DETAILS
- Donor egg IVF cycle initiated. Donor stimulated and eggs retrieved
- Husband’s semen sample frozen in advance to accommodate travel constraints
- Fertilisation done in the lab. 10 Grade A embryos were produced and frozen at blastocyst stage
- First frozen embryo transfer attempted in April 2025. Transfer was technically difficult due to intrauterine adhesions. Cycle was negative
- Hysteroscopy performed. Roomy cavity noted with fundal adhesions, which were cut using scissors. PRP was instilled into the cavity to support endometrial regeneration
- Hysteroscopy confirmed direct entry from vaginal introitus into the uterus, reconfirming cervical absence
- Second frozen embryo transfer done in August 2025. Beta hCG doubling was good. Pregnancy confirmed
- Small uterine fibroid noted. Gestational diabetes developed due to advanced maternal age and was managed with medication
- At 12 weeks, after genetic markers of the foetus were cleared, elective laparoscopic cervical cerclage was performed. The knot was tied as high as technically possible on the lower uterine segment
- Sugar levels stabilised with ongoing medical management
- Pregnancy monitored closely through all three trimesters
- Patient delivered at 37 weeks. A healthy 2.2 kg male baby was born, cried immediately, and required no NICU admission
PROCEDURE FACTS
| PROCEDURE | Donor Egg IVF with FET, Hysteroscopic Adhesiolysis + PRP, Laparoscopic Cervical Cerclage |
| EMBRYOS GENERATED | 10 Grade A blastocysts |
| CERCLAGE TYPE | Laparoscopic cervical cerclage (lap surclash), elective, at 12 weeks |
| GESTATION AT DELIVERY | 37 weeks |
| BABY OUTCOME | Healthy male, 2.2 kg, immediate cry, no NICU stay |
OUTCOMES AT A GLANCE
| Conception | Achieved on second FET after hysteroscopy and PRP |
| Pregnancy Continuation | Successfully carried to 37 weeks with cerclage |
| Baby Outcome | Healthy male, 2.2 kg, immediate cry, no NICU stay |
| Maternal Outcome | Stable. GDM controlled. No intraoperative or delivery complications |
| Patient Satisfaction | Very high. Long-awaited parenthood achieved after repeated loss |
| Complications | None reported |
PATIENT FEEDBACK
Google Review ★ ★ ★ ★ ★ 5.0 “We had lost our daughters. Then we lost the baby at 8 months. I did not think any hospital would take my case seriously at this stage. Dr. Mohit Saraogi explained every step, told me what was possible and what was not, and did not hide anything. Today I have my baby in my arms. I will be grateful to the Saraogi team forever.” Profile: Female | 40 years | Rural patient | Referred to Mumbai Procedure: Donor Egg IVF, Hysteroscopy, Laparoscopic Cervical Cerclage | Saraogi Hospital, Mumbai | 2025 Clinician: Dr. Mohit R. Saraogi | Saraogi Hospital & IRIS IVF Centre Note: Due to privacy regulations, we cannot display the patient’s name. This feedback has been shared with the patient’s written consent. |
POST-PROCEDURE CARE AND RECOVERY
- Strict bed rest advised in the first trimester after FET and post-cerclage
- GDM monitored with regular blood sugar checks and medication adjustments
- Avoid heavy lifting, travel, and physical strain through the second trimester
- Regular follow-up every 2 to 3 weeks until 28 weeks, then weekly monitoring
- Growth scans, Doppler studies, and foetal well-being tests as per high-risk pregnancy protocol
- Cerclage remained in place until planned delivery
- Emotional support and counselling offered throughout pregnancy, given prior losses
- No smoking, no unsupervised medication, and full hydration advised
RECOVERY TIMELINE
| Week 1 to 4 after FET | Beta hCG rising well. Early viability scan confirmed pregnancy. |
| Week 5 to 12 | Close monitoring. GDM diagnosed and medication started. |
| Week 12 | Elective laparoscopic cervical cerclage performed. Knot tied high. |
| Week 13 to 28 | Stable progress. Sugars controlled. Regular growth scans done. |
| Week 28 to 37 | Weekly monitoring. Cerclage intact. Foetal growth within range. |
| Week 37 | Delivery. Healthy 2.2 kg male baby. No NICU admission. Mother stable. |
DISCLAIMER: This case study is for informational purposes only and does not constitute medical advice. Individual results may vary. Consult a qualified fertility specialist before undergoing any procedure. Patient feedback published with written consent. Patient identity withheld per confidentiality guidelines.
